About every two seconds, someone in the United States needs blood. That is a lot of blood to transfuse from donors to patients. The faults and failures of early transfusions have significantly helped shape how blood transfusion procedures work today. Before anyone understood blood, scientists knew that blood was a life force flowing through us all.
To harness the power of blood and infuse it into another person, usually someone sick or dying. Patients would usually drink the blood, which did not affect them. The idea of a blood transfusion didn’t occur until William Harvey’s 1628 discovery that blood circulates through the body in one direction. Then, scholars and doctors realized that transfusions were a possible method of rejuvenating the sick.
What is a blood transfusion?
A blood transfusion is a standard procedure that involves taking blood from one person, the donor, and giving it to someone who requires more blood. The most common reason for a blood transfusion is to address a shortage of red blood cells. Red blood cells are necessary for carrying oxygen around the body. Sometimes this happens because the bone marrow, which produces red blood cells, can’t make enough of them.
When is a patient transfused? It depends on what’s going on with the patient, their vital signs, and how they tolerate that low blood level. Recent guidelines by the American Association of blood banks recommend transfusing blood when hemoglobin levels fall to 7 to 8 grams per deciliter.
Normal hemoglobin level:
- Male, 14 to 18 grams per deciliter.
- In females, it’s 12 to 16 grams per deciliter.
How do blood transfusions work?
Blood transfusions involve transferring blood or components from a donor to a recipient. They commonly replace lost blood, restore blood volume, or provide specific blood components necessary for various medical conditions. Here’s a general overview of how blood transfusions work in the body:
Compatibility Testing: The recipient’s blood is tested to determine the blood type and Rh factor before a blood transfusion. This is crucial to ensure compatibility between the donor and recipient blood types to prevent adverse reactions.
Donor Selection and Collection: Compatible blood is selected from a donor or blood bank once the recipient’s blood type is determined. The donor blood is collected using sterile techniques, typically from a vein in the arm.
Blood Component Preparation: Blood can be transfused in different forms, depending on the recipient’s specific needs. It can be transfused as whole blood, red blood cells, platelets, or plasma. Blood components may also undergo processing, such as leukocyte reduction or irradiation, to remove specific components or reduce the risk of complications.
Transfusion Process: The collected blood or components are administered to the recipient through an intravenous (IV) line. The transfusion is typically carried out slowly and closely monitored to ensure safety and detect adverse reactions. The transfusion rate may vary depending on the recipient’s condition and the transfused blood component.
Compatibility and Immune Response: The compatibility of the donor blood with the recipient’s blood type is crucial to prevent adverse reactions. Incompatible transfusions can trigger an immune response in which antibodies in the recipient’s blood recognize and attack the donor blood cells. This can result in severe reactions, such as hemolysis (destruction of red blood cells), fever, chills, or more severe allergic responses.
Monitoring and Response: Throughout the transfusion process, the recipient’s vital signs, including heart rate, blood pressure, and oxygen levels, are closely monitored. If any adverse reactions or complications arise, appropriate interventions, such as stopping the transfusion or administering medications, may be implemented to manage the situation.
Post-Transfusion Care: After the transfusion, the recipient’s response is monitored, and any post-transfusion symptoms or complications are managed accordingly. In some cases, additional blood tests may be performed to evaluate the effectiveness of the transfusion or monitor for potential complications.
Blood carries oxygen and nutrients to tissues, removing carbon dioxide and other waste products. It also helps fight infection and heal wounds. Blood consists of a liquid portion and cellular components. In the plasma liquid, nutrients, hormones, clotting factors, and other chemicals are dissolved. The cellular components are suspended in the plasma.
- They consist of red blood cells that transport oxygen and carbon dioxide.
- White blood cells fight infection.
- Platelets are small subcells that help the blood clot.
Blood cells are made in the bone marrow, a soft tissue housed inside many bones. A blood transfusion uses donor blood to replenish:
- Red blood cells.
- White blood cells.
- Platelets.
- Clotting factors.
- Plasma.
Whole blood circumstances that may require a blood transfusion include:
- Blood loss due to trauma.
- Heart or other major surgery.
- Organ transplants.
- Bleeding disorders such as Hemophilia.
- Severe anemia, including sickle cell Anemia.
- Treatment for leukemia or other types of cancer.
- Disorders that destroy blood cells or bone marrow.
- Rh incompatibility in newborn babies.
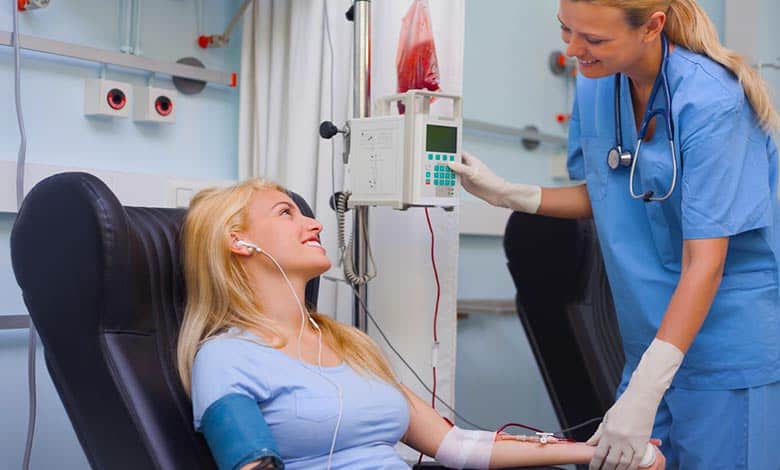
A bag containing the donor blood will be hung nearby to begin the transfusion, and the intravenous needle will be inserted into a vein in the hand or arm. The blood will drip slowly through a tube attached to the IV needle allowing it to run through the vein into the bloodstream. The donor’s body temperature, heart rate, breathing, and blood pressure will be monitored throughout the transfusion.
After the bag is empty, another bag will be attached to the IV tube if the patient requires more blood. When the transfusion is completed, the needle will be removed. After the transfusion, the doctor will monitor vital signs to avoid an adverse reaction. The patient may be given an emergency diuretic to reduce swelling or fluid retention.
By the end of the 17th century, physicians used quills as needles and silver pipes to transfer blood from a donor to a recipient. But the donor was usually an animal. No one knew that animal blood cells were incompatible with human blood. It wasn’t. Obstetrician James Blundell started using human blood to replace blood lost in childbirth in the early 1800s. That transfusion began working, at least some of the time.
Physician Karl Landsteiner discovered why some blood transfusion patients lived and others died. A line of inquiry led him to discover the ABO blood type groups in 1901. Landsteiner’s groundbreaking work helped classify blood into four categories: A, B, AB, and O. The antigens and antibodies define these on the cells.
People with type A blood, for example, have the A antigen on the surface of their red cells. Their bodies won’t produce anti-A antibodies. So if any type A blood is introduced into that person’s body, it won’t recognize the new cells as foreign and won’t attack them. But if type B blood is injected into a type A blood person, the anti-B antibodies on the donated blood will be seen as foreign. The host’s body will reject the transfusion.
Another factor for rejection comes down to a protein on the surface of red blood cells called the Rhesus or Rh factor. Blood cells either possess the protein. It means that Rh is positive or negative. These factors combine to make eight blood types.
All of this is important because blood type determines compatibility with a donor. The red blood cells of people with type O blood have A or B antigens on their surface, making them universal donors. People with type AB blood don’t produce any antibodies. So they are universal recipients. But everyone else is only compatible with their specific type.
So knowing what we’ve learned over centuries of trial and error, blood transfusions have become simpler. There’s no need for a living donor. Instead, donated red blood cells can be stored for 42 days. It means a patient in need is given an IV and a bag of blood to replenish what they’re missing or restore blood lost in an accident.
Blood transfusion procedure
A blood transfusion is a straightforward procedure that a nurse carries out. At first, Donar will need to sign a consent form. Before a blood transfusion, a nurse or doctor will go through this. They can ask as many questions as they like. A nurse or doctor will take a small blood sample to check the blood type. Donors must be given blood compatible with the receiver’s blood type. So donors must be correctly identified at each stage of the blood transfusion.
Then donors will be asked to state their full name and date of birth. Some people will be given a card to say they can only get specific blood types when they have a blood transfusion.
Donar can sit up or lie down during transfusion at roughly 15-minute intervals. The blood is usually given through a tiny tube called an intravenous line inserted directly into a vein in the arm using a fine needle. The insertion may cause slight discomfort, but the donor shouldn’t feel anything during the transfusion. Giving the patient each blood bag may take up to four hours.
However, this can be safely speeded up when necessary or urgent. The patient may be given more than one blood bag as part of treatment. Blood transfusions are very safe, and it has many benefits. Donate your blood and save a life.
More Articles:
History Of The Blood Evolution
How Do The Neurotransmitters Work?
References:
“Blood Transfusion | National Heart, Lung, and Blood Institute (NHLBI).”
Adams RC, Lundy JS. “Anesthesia in cases of poor surgical risk. Some suggestions for decreasing risk”.
“Five Things Physicians and Patients Should Question,” Choosing Wisely: an initiative of the ABIM Foundation, American Association of Blood Banks.